Moa Jamir
Dimapur | April 26
Public hospitals continue to serve as the backbone of healthcare in Nagaland, with the state recording far higher dependence on government health facilities than the national average for treatment and hospitalisation, according to the latest National Sample Survey (NSS) 80th Round on Household Social Consumption: Health.
The nationwide survey, conducted between January and December 2025, also indicated that while Nagaland households spend less than the national average on hospital admissions, many continue to face a heavier burden for routine, non-hospitalised treatment.
Govt hospitals remain primary pillar
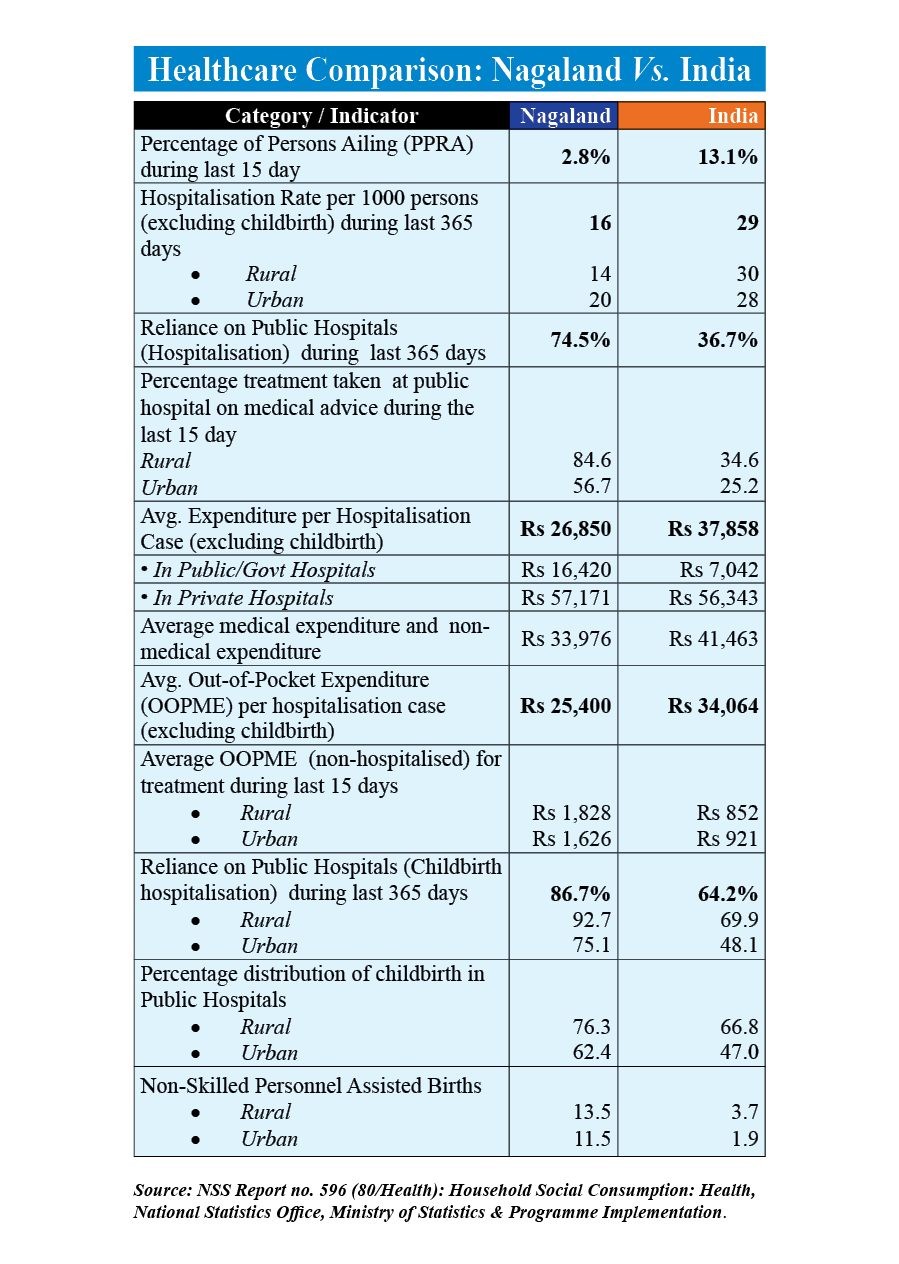
The survey found that 74.5% of all hospitalisation cases in Nagaland were treated in public hospitals, more than double the national average of 36.7%.
Private institutions accounted for 25.6% in the state, compared to 60.3% nationally.
In rural Nagaland, dependence on government hospitals was even higher at 78.2%, reflecting the central role of the public health system for communities with limited access to private care.
For non-hospitalised treatment as well, public institutions remained the first point of care. In rural Nagaland, 84.6% of treated ailments on medical advice during the last 15 days of the survey were handled by government hospitals or public facilities, the highest share among states in India. The all-India average was 56.7%.
In urban areas, the figure stood at 56.7%, still well above the national urban average of 25.2%.
Incidentally, the survey also highlighted that a substantial share of treatment in urban Nagaland was sought from informal healthcare providers, accounting for 17.7%.
Lower illness reporting, lower hospitalisation
Nagaland recorded a Persons Responded as Ailing (PPRA) rate of 2.8%, against the national average of 13.1%. Among persons aged 60 years and above, the state reported 13.5%, compared to 43.9% nationally.
The overall hospitalisation rate (excluding childbirth) stood at 16 per 1,000 persons, lower than the national average of 29.
Urban Nagaland recorded a higher rate (20) than rural Nagaland (14), indicating better access to inpatient services in towns than in villages.
Lower hospitalisation costs, higher everyday burden
In what could be an indication of universal health schemes such as CMHIS (Chief Minister Health Insurance Scheme), Nagaland households spent less than the national average on hospital admissions.
The average out-of-pocket medical expenditure per hospitalisation case stood at ₹25,400, compared to ₹34,064 nationally. Average total medical expenditure per hospitalisation case in the state was ₹26,850, against ₹37,858 nationally.
However, the burden was heavier for routine care.
The average out-of-pocket expenditure for non-hospitalised treatment in rural Nagaland was ₹1,828, more than twice the national rural average of ₹852. The state average stood at ₹1,626.
Besides, expenditure at private doctor/clinic was shown to be ₹13,341.
This suggests that while government hospitals may be cushioning families against major medical expenses, households could still be paying heavily for medicines, consultations, travel and minor treatment.
High institutional delivery, home deliveries persist
Government institutions also carried the bulk of childbirth care in Nagaland. The survey found that 86.7% of childbirth-related hospitalisation cases in the state took place in government institutions, compared to about 64% nationally, while private institutions accounted for 13.3%, against 34.8% nationally.
In rural Nagaland, 76.3% of childbirths occurred in government facilities, while only 6% took place in private institutions. In urban areas, government facilities accounted for 62.4%, with private institutions handling 20.7%.
However, childbirths attended by unskilled personnel remained notably high at 13.5% in rural areas and 11.5% in urban areas, compared to national averages of 3.7% and 1.9% respectively.
The figures may indicate continuing challenges linked to remoteness, transport, cultural preferences, emergency access or gaps in last-mile maternal healthcare outreach.



.jpg)


